
Patellofemoral Pain (PFP) is one of the most common injuries runners experience. In fact, it is one of the most common conditions we see in outpatient physical therapy! So, if you’re experiencing generalized knee pain, participating in a running program (shout out to our #RunStrong participants), or are just curious about the underlying issues associated with a very prevalent condition, look no further!
PFP is typically described as knee pain in the front of the knee that involves the patella (knee cap). Women typically experience PFP more often than men, and common symptoms include pain that is felt with activities that load your patellofemoral joint, such as climbing stairs, squatting, and jogging. Although this description may seem simple, or even a little vague, PFP can be very complicated to treat because the exact cause of it is not completely understood. A lot of research has been dedicated to understanding this condition more, and though we don’t know exactly why PFP arises, we do have a better understanding of how to treat it.
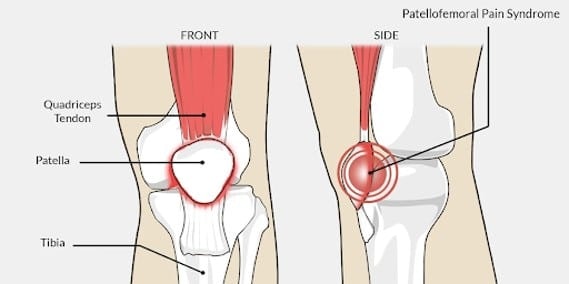
The best evidence and research out there suggest there are a few key things to address in treating PFPS: 1. glute and quad strength, 2. lower body control, and 3. activity frequency/quantity.
Glute and quadriceps strength are very important to address if you’re experiencing PFP. Studies have shown that people with PFPS have significant hip abduction, hip external rotation, and knee extension strength deficits. It is unknown whether these deficits are the cause of PFP or a product of PFP (chicken vs. egg??). However, we do know that by strengthening the muscles that perform those actions, ie, your quads and glutes, you’ll see an improvement in pain levels and function over time. If you’re experiencing PFP, or even want to work on injury prevention, check out the strengthening exercises in the video about PFP below!
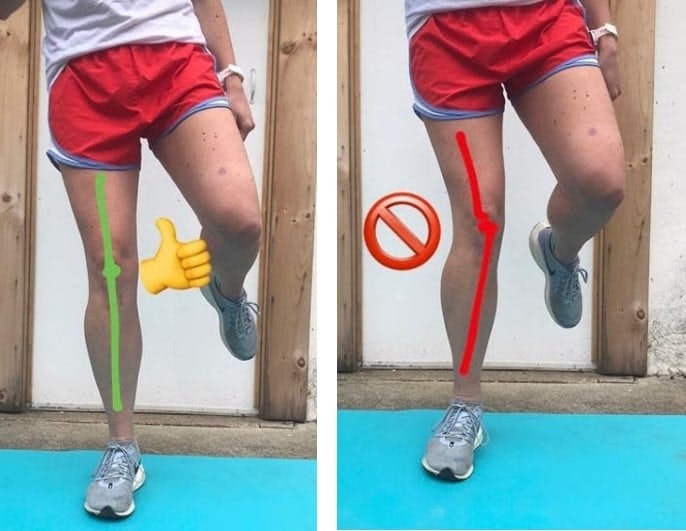
Lower body control is another key aspect to work on. Whether it’s habit, or the weak muscles I just mentioned, many runners and well-trained people struggle to keep their knees in the best position. The less favorable position, otherwise known as “knee valgus”, predisposes you to injury and even contributes to developing PFP! Research has shown that as the amount of valgus increases, the amount of stress on your patellofemoral joint increases, which can cause increased irritation in that area. Practicing activities with good form (see photo below) and lots of repetition can help you form better habits and strength so that when you’re doing dynamic activities, you keep your knee in a better position and put less of a load through your patellofemoral joint. Try some of the exercises below and see how you do!!
Last on our list: activity frequency and quantity. PFP is often described as an overuse syndrome, meaning ramping up your mileage or activity too fast and putting more stress on the body than your tissues can tolerate at that moment. There are a few things you can do if you think you’re overdoing it. Adjusting your run program is a good place to start. Add a few more rest days, decrease your mileage if you can and do some fun cross-training instead, target strength deficits that can be contributing to your pain. A rule of thumb that I live by is the 10% rule: don’t increase your weekly mileage by more than 10% from one week to the next. If you follow a guideline that helps you control your training, you put yourself at less of a risk for overuse injuries by making sure your body is able to tolerate the repetitive stresses you’re putting on it. The more you know!!
As I’ve mentioned, PFP is a pretty complicated condition; these key components are just a few adjustments among many that can be made. If you’re feeling some pain in your knee and these symptoms ring a bell, or you want to work on prevention, reach out to your favorite 3DPT physical therapist!! We can break down your movement and analyze your training schedule to help you figure out just what you need to do to beat that PFP. You got this, and happy running!!
Citation:
Barton CJ, Lack S, Hemmings S, et al. The ‘Best Practice Guide to Conservative Management of Patellofemoral Pain’: incorporating level 1 evidence with expert clinical reasoning. British Journal of Sports Medicine 2015; 49:923-934.
Categorized as: Blog Run Strong,Knee,Run Strong with 3DPT,Sports Injury